
Philosophy Department
University of Waterloo
Waterloo, Ontario, N2L 3G1
pthagard@watarts.uwaterloo.ca
© Paul Thagard, 1997
To go directly a particular section of this paper, click on a section title below.
To return to the Science and Disease Articles Table of Contents page, click here.
My description of the cognitive processes involved in the discovery, development, and acceptance of the bacterial theory of ulcers might have left the impression that science is all in the mind (Thagard, forthcoming-b). But only part of the story of the bacterial theory of ulcers is psychological. This paper discusses the important role of physical interaction with the world by means of instruments and experiments, and the equally important role of social interactions among the medical researchers who developed the theory. The main questions I want to answer are the following:
1. What instruments contributed to the development and acceptance of the new theory?
2. What kinds of experiments contributed to the development and acceptance of the new theory?
3. How did theorizing and experimentation interact in the development of new experiments and hypotheses?
4. How did social processes such as collaboration, communication, and consensus contribute to the development and widespread acceptance of the bacterial theory of ulcers?
I conclude with a sketch of science as a complex system of interacting psychological, physical, and social processes.
Both the discovery and the evaluation of the bacterial theory of ulcers would have been impossible without several kinds of scientific instrument that make possible the examination of bacteria and the gastrointestinal system. Microscopes, endoscopes, and other technologies played crucial roles in investigations concerning Helicobacter pylori and ulcers.
Because bacteria are very small, typically 0.1 to 5 microns (micrometers), they cannot be observed by the naked eye. Around 1600, spectacle makers in Holland discovered how to produce and combine lenses to increase magnification of small objects. In approximately 1673, a Dutch draper, Antony van Leeuwenhoek, became interested in the new devices. He began building his own single-lens microscopes, achieving magnifying power as high as 275X with resolving power approaching 1 micron (Brad bury, 1968). Leeuwenhoek described his observations in letters to the Royal Society of London, and in 1676 reported finding "little animals' in water (Dobell 1958, p. 133). These bacteria were much smaller than the protozoa that he had previously observed, but their medical significance was not appreciated until the work of Pasteur in the mid-nineteenth century.
Gastric spiral bacteria were microscopically observed as early as the 1890s, and in the 1970s Steer and Colin-Jones (1975) reported the co-occurrence of gastric bacteria and ulceration.. They were unsuccessful, however, in attempts to culture the bacteria, which they identified as Pseudomonas aeruginosa. In 1979, Dr. Robin Warren was using an Orthoplan optical microscope at 250x magnification to examine histologic sections from patients with gastritis. He noticed the unexpected presence of spiral bacteria, and then used an oil immersion microscope capable of 1000x magnification to examine them more closely. In order to observe the morphology of the bacteria more clearly, he requested a Warthin-Starry silver stain on gastric biopsies and was able to see a large number of spiral organisms. He had previously used this kind of stain for observing the spirochetes that are responsible for syphilis. Staining of bacteria, which originated with Herman Hoffman in 1869, makes possible much clearer observation of their structure (Bulloch 1979).
All subsequent experiments observing the correlation of the bacteria and various diseases, as well as the experiments finding that eradicating the bacteria can cure diseases such as gastritis and ulcers, used microscopes to determine the presence or absence of bacteria in the gastric biopsies. Without microscopes, bacteria would never have been discovered, and the bacterial theory of ulcers would never have been developed and accepted.
Although most of the clinical research involving Helicobacter pylori has been performed using optical microscopes, electron microscopes proved very useful in identifying the detailed morphology of the newly discovered species of bacteria. In 1982, just after the first cultures of H. pylori were produced, Barry Marshall delivered specimens to an electron microscopist, Dr. John Armstrong, who produced the first electron micrographs of the bacteria (Marshall, 1989). Armstrong identified the essential morphological features, four or five sheathed flagella, that differentiated the gastric spiral bacteria from the species Campylobacter jejuni. Subsequent investigations, using electron microscopes and other technologies such as RNA sequencing, provided evidence that the bacteria did not belong in the genus Campylobacter and led to the naming of a new genus, Helicobacter (Goodwin and Worsley, 1993). Without these instruments permitting much more detailed observation of the structure and properties of the gastric bacteria, the conceptual change that produced a reclassification of the bacteria would not have been possible. Figure 1 is a photograph of H. pylori.

Figure 1. Microscopic photograph of H. pylori (arrows).
Source: http://www.pds.med.umich.edu/users/greenson/HP-SILVER.GIF. Used by permission of Joel K. Greenson, M.D.
Production of the gastric biopsy slides that investigators look at with microscopes employ an instrument that only came into general use in the 1960s, the fiber optic endoscope. Endoscopes, such as gastroscopes, proctoscopes, and esophagoscopes, are tubular instrument used to examine the inside of body cavities. After unsuccessful 19th-century experiments with candles and incandescent lamps as light sources, the first usable straight gastroscope was produced in 1911 (Hirschowitz 1993). But the available instruments were difficult to use and often did not allow adequate inspection of the stomach. A semiflexible gastroscope produced in 1932 was still uncomfortable for patients and limited in what portions of the stomach it could be used to visualize. Endoscopy was rarely used for diagnosis of upper gastrointestinal tract diseases, which depended instead on barium x-rays.
In the 1950s, a new technology for transmission of information became available. Hopkins and Kapany (1954) designed a flexible fiberscope that uses glass fibers encased in a cladding to direct light along a curved path. Fiber optics have since become the main medium for carrying all types of telecommunications, but one of their first applications was the manufacture of endoscopes for medical exploration. In 1957, Basil Hirschowitz and his colleagues produced the first fiber-optic gastroscope, and such instruments were in clinical use by the early 1960s. Improved instruments included biopsy channels for taking tissue samples from the stomach and, after 1983, video screens on which the endoscopist and others can observe the stomach.
By the 1970s, endoscopy had become a standard technique for gastroenterologists, who, by inserting a tube with fiber optics down the throat of patient, can view the inside of the stomach. An ulcer is immediately visible as a sore or hole in the lining of the stomach (gastric ulcer) or as a sore on the upper part of the intestine (duodenal ulcer). Endoscopy not only makes possible identification of ulcers, it also enables gastroenterologists to take samples of stomach tissue by means of a miniature pincer attached to the end of the endoscope. They can thus pass tissue samples to pathologists for further examinations. Robin Warren's observations of bacteria in stomach tissue in the late 1970s were done on samples obtained via endoscopy. Figure 2 shows an early gastroscope.
Endoscopy has also played a crucial role in all the experiments that have contributed to the acceptance of the bacterial theory of ulcers. Definitive diagnosis of a peptic ulcer is made by endoscopic observation of lesions, and endoscopically-gained samples are crucial for determining the presence or absence of Helicobacter pylori. The early experiments described below that found a correlation between the presence of bacteria and ulcers, and the later more conclusive experiments that showed that antibiotics can eradicate bacteria and cure ulcers, all depended on internal examination and tissue sampling using endoscopes. Without endoscopy to provide stomach samples, the bacterial theory of ulcers would never have been discovered or validated.

Figure 2. A modern fiber-optic endoscope.
Source: http://www.mindspring.com/~dmmmd/atlas_1.html. Used by permission of David M. Martin, M.D.
Originally, the only way to diagnose infection was by endoscopic biopsy of the gastric mucosa. But David Graham and his colleagues designed a non-invasive detection method based on the fact that H. pylori produces large amounts of urease that buffers it from gastric acid (Graham et al., 1987; see also Marshall et al. 1991). Patients suspected of having H. pylori in their stomachs are given a small quantity of urea containing an isotope of carbon. If urease is present, it reacts with the urea to form carbon dioxide containing the isotope, which is detected by having the patient breath into a balloon. Patients with stomach distress can be diagnosed as having H. pylori infection without undergoing the expensive and somewhat unpleasant experience of endoscopy, and immediately treated with antibiotics. Cutler et al. (1995) report that urea breath tests are as effective as endoscopic biopsy for diagnosing infection. Urea breath tests were not important in the discovery or validation of the bacterial theory of ulcers, but they promise to be of increasing importance in future treatment of gastritis and ulcers (1).
The centrality of the use of microscopes, endoscopes, and other instruments makes it clear that gastroenterologists and microbiologists are not disembodied researchers spinning ideas in their heads removed from contact with the world. While their use of instruments is guided by their conceptual systems, those systems do not determine the observations that researchers bring about through instrumental interventions with microorganisms and bodily tissues. Scientific change derives from technology as well as from psychology. Formation of the initial concept of gastric spiral bacteria and refinement of the concept into Campylobacter pyloridis and finally Helicobacter pylori required physical processes by which researchers took stomach samples using endoscopes and observed the extracted bacteria using optical and electron microscopes. These physical processes are much more complex than simple sensory observation, since substantial skill and training are required to obtain and interpret the results of endoscopy and microscopy. Nevertheless, the physical processes of instrument use and the mental processes of interpretation of the data provided by the instruments yield substantial agreement across time and across researchers. But agreement arises not merely because of the isolated use of instruments, but also because of the systematic conduct of medical experiments.
Recent philosophy and history of science has paid increasing attention to the role of experiment in scientific research (see, for example, Ackermann 1985, Galison 1987, Gooding 1990, and Hacking 1983). . Attention to experiment has valuably redressed an imbalance toward theory in previous science studies, but almost all of the investigations have concerned experiments in physics. Medical experimentation takes on quite different forms, which I now want to describe with particular reference to the experiments that were important to the development and acceptance of the bacterial theory of ulcers.
Hennekens and Buring (1987) describe six kinds of studies that can be used to investigate the distributions and causes of diseases.
1. Correlational studies use data from entire populations to compare disease frequencies between different groups during the same period of time or in the same population at different points of time. For example, there is a positive correlation across countries between high consumption of meat and colon cancer. Such correlational studies can be a useful source of hypotheses about the causes of diseases, but are weak for evaluating causal claims because of unknown effects of other variables.
2. Case reports and case studies consist of detailed descriptions of one or more patients with a particular disease. For example, the occurrence of a particular kind of pneumonia in five young, previously health young men in Los Angeles in 1980 suggested the existence of a previously unknown disease (AIDS) and led to the conjecture that the cause of the disease might be related to sexual behavior.
3. Cross-sectional surveys are large studies that collect extensive information from individuals at a particular point in time. They make possible calculation of the frequencies of various diseases in relation to age, sex, race, socioeconomic variables, medication use, cigarette smoking, and other risk factors. While such studies can be suggestive about the causes of disease, they are never definitive, since causes and effects are difficult to disentangle. For examples, when individuals with cancer are found to have lower levels of serum beta-carotene, it is not clear whether the lower levels are a cause or an effect of the cancer.
Hennekens and Buring (1987) contrast these three kinds of descriptive study with analytic studies in which an investigator assembles groups of individuals in order to make an explicit comparison of the risk of disease of those exposed to a factor with those not exposed.
4. Case-control studies select a group of patients that have a disease and compare them with a control group of patients without the disease. For example, a group of patients with a particular kind of cancer can be compared with a group of similar patients without cancer. The comparison can look at various potentially relevant variables such as diet, smoking, medication use, and so on.
5. Cohort studies differ from case-control studies temporally: subjects are classified on the basis of presence or absence of exposure to a factor and then followed over time to determine the comparative development of disease in each exposure group. For example, in the early 1950s the Framingham Heart Study established a cohort of more than 5000 people identified with respect to medical history, cigarette smoking, and a variety of laboratory variables. Reexamination of members of the cohort at regular intervals has identified numerous risk factors for cardiovascular disease.
6. Intervention studies (clinical trials) are a special kind of cohort study in which the exposure status of the individuals is randomly determined by the investigator. The advantage of random assignment to exposure and non-exposure conditions is that it controls for the effects of other risk factors, both recognized and unrecognized. For example, randomly assigning patients with hypertension into groups receiving a medication and not receiving it can provide evidence of the effectiveness of the medication. Hennekens and Buring (1987, p. 26-27) remark that "when well designed and conducted, intervention studies can indeed provide the most direct epidemiologic evidence on which to judge whether an exposure causes or prevents a disease."
Experimental work on ulcers and bacteria moved through increasing stages of sophistication, from case studies to a cross-sectional survey to intervention studies. Warren's noticing of an association between spiral bacteria and gastritis was based on 135 gastric biopsy specimens collected between 1979 and 1982 (Warren and Marshall, 1983). In July, 1981, Warren gave Marshall a list of 25 patients in whom large numbers of gastric spiral bacteria were present, but Marshall's examination of the patients' case notes did not reveal any characteristic clinical features (Marshall, 1989). In September, 1981, Marshall used the antibiotic tetracycline to treat a patient with abdominal pain of unknown origin, and the patient's symptom's and gastritis were completely resolved. Marshall and Warren then began a more systematic investigation of the clinical significance of the bacteria.
Between April and June, 1982, Marshall and his colleagues collected biopsy specimens from 100 patients who had been scheduled for endoscopy. Warren received the biopsies and examined them for the presence of the bacteria. Marshall coded the endoscopy reports for the 100 patients to record occurrences of gastritis and gastric and duodenal ulcers. Questionnaires, endoscopy reports, and microbiology results were coded independently in separate departments, and complete results for individual patients were not known until the statistician had received all the data (Marshall and Warren, 1984). In October, 1982, Marshall received printouts from the statistician and immediately noticed a strong association between gastritis and the gastric spiral bacteria (Marshall, 1989). Only later did he notice that all 13 patients with duodenal ulcer also had the organism. When Marshall and Warren reported these associations in Lancet, they concluded (1984, p. 1314): "Although cause-and-effect cannot be proved in a study of this kind, we believe that pyloric campylobacter [later, H. pylori] is aetiologically related to chronic antral gastritis, and, probably, to peptic ulceration also." Intervention studies were needed before stronger claims about causal relations could be made convincingly. Marshall et al. (1985) reported a replication at Fremantle Hospital of the results of the 1982 study, again finding that bacterial infection strongly correlated with both gastritis and gastric ulcer. They also reported on the basis of in vitro studies that the bacteria were sensitive to numerous antibiotics, including penicillin, erythromycin, and tetracycline. This sensitivity made possible the cure-based intervention studies described in the next section.
The purpose of the 1982 experiment was not just to determine the medical significance of the bacteria but also to learn more about their nature. From each patient, two biopsy specimens were taken, one sent for microscopic examination to Robin Warren, the other transported to the microbiology lab in nutrient broth. After many tries, the organism was cultured for the first time in April, 1982. Sections were also sent to Dr. John Armstrong, the electron microscopist at Perth General Hospital, for ultrastructural examination. Thus the 1982 experiment involved all the major technologies describe in the last section: optical microscopes, light microscopes, and endoscopes. It also required the various technologies developed in the nineteenth century for culturing and observing bacteria, such as growth media, incubators, and stains.
As Marshall and Warren (1984) explicitly noted, the 1982 experiment was not sufficient to establish a causal relation between the gastric spiral bacteria and gastric diseases. To establish causality, two kinds of intervention studies were relevant: giving people the bacteria and seeing if they came down with gastritis or ulcers, and eliminating the bacteria in people with gastritis or ulcers to see if doing so eliminates the diseases. Obviously, it would be ethically objectionable to conduct the first kind of study, but in 1984 Barry Marshall performed the experiment on himself. After gastroscopy found no bacteria present in his stomach, he swallowed a three-day culture of the bacteria, and after a week suffered from vomiting, headache, and putrid breath. After ten days gastroscopy and microscopy found that spiral bacteria had established themselves in Marshall's stomach. On the fourteenth day, Marshall began taking the antibiotic tinidazole and his symptoms resolved within twenty-four hours. Marshall (et al., 1985) described this experiment as an "Attempt to fulfil Koch's postulates for pyloric campylobacter" for gastritis. It is standard in medical microbiology to show that a microbe causes a disease by isolating the microbe from an infected animal and transferring it to a new animal that contracts the disease (see Thagard, forthcoming-b). Since early attempts to cause gastric disease in non-human animals using H. pylori had failed, Marshall's self-experiment was an important part of the evidence that the bacteria cause gastritis. It did not, however, address the question of whether the bacteria cause gastric ulcers, since Marshall was cured before an ulcer could develop.
Between April, 1985, and August, 1987, Marshall and numerous colleagues at Royal Perth Hospital examined 100 consecutive patients with both duodenal ulcer and H. pylori infection to see whether eradication of the bacteria affected ulcer healing or relapse (Marshall et al., 1988) (2). This experiment was double-blind, in that histology and microbiology findings were concealed from both the patients and the doctors managing them. Patients were randomly assigned to receive either the antacid cimetidine or colloidal bismuth subcitrate, and either tinidazole or a placebo. The four treatment groups were thus cimetedine+tinidazole, cimetidne+placebo, bismuth+tinidazole, and bismuth+placebo. Bismuth+tinidazole was by far the most effective combination, clearing the infection in 20 of 27 patients. After 10 weeks, patients underwent endoscopy, and healing of ulcers had taken place in 92% of patients in whom H. pylori were not detected, compared to only 61% of patients with persistent H. pylori. Marshall et al. (1988, p. 1441) concluded: "Our results imply that C pylori [H pylori] is the most important aetiologic factor so far described for duodenal ulcer." Many other researchers have done similar experiments that show that various kinds of antibiotic therapy are effective at healing both duodenal and gastric ulcers and at preventing their recurrence (Thagard forthcoming-b). The accumulated evidence provided by these intervention studies is such that in 1995 Barry Marshall was awarded the highly prestigious Albert Lasker clinical medical research award "For the visionary discovery that Helicobacter pylori causes peptic ulcer disease." I note again that endoscopes and microscopes were essential ingredients in these intervention experiments.
I have summarized the early experiments whose results Marshall and Warren reported in publications, but looking only at published reports ignores the importance of small pilot experiments that scientists use to determine if they are on the right track before investing more resources in larger studies. Before Marshall and Warren did the 1982 study involving 100 patients, they did a smaller preliminary study with 20 patients who underwent endoscopy. Similarly, in 1983, before beginning a major study on the effects of H. pylori eradication on ulceration, Marshall did a pilot study in which he found that ulcer patients treated with bismuth had a substantially lower relapse rate than those treated with Tagamet. This study provided early support for the hypothesis that bismuth kills bacteria, thereby healing gastritis and preventing ulcer relapse. Pilot studies are not probative in themselves, but play an important role in determining what large-scale experiments are deemed worth performing.
The experimental developments concerning ulcers and bacteria belie several simplistic pictures of how science works. Experiment and theory interact in ways more complex than any of the following caricatures describes:
1. Inductivist: scientists do experiments to collect data and then generalize the results. Good hypotheses and theories are derived from experimental results.
2. Hypothetico-deductivist: scientists start with hypotheses and then do experiments to test them. If the experiments come out as predicted, the hypotheses are confirmed; otherwise, the hypotheses are refuted.
3. Social constructivist: experiments are part of the social construction of scientific facts.
The inductivist picture fits best with Marshall's and Warren's 1982 experiment where they sought to find out whether gastric symptoms and diseases correlate with the occurrence of gastric spiral bacteria. This experiment was not designed to test any specific hypothesis about the medical role of H. pylori. Nevertheless, the experiment did not operate in a theoretical vacuum either: Marshall did not know what diseases the bacteria might be associated with, but he did suspect, presumably by analogy with the disease-causing effects of some other kinds of bacteria, that H. pylori might be the cause of some diseases. The design of the 1982 experiment specifically looked for associations between presence of the bacteria and specific diseases of interest: gastritis, gastric ulcer, duodenal ulcer, and other stomach abnormalities. Marshall and Warren were neither simple-minded empiricists, merely collecting experimental data, nor theory-blinded deductivists, trying to confirm their own predictions. At this stage of the investigation, they had no clear predictions to test.
In contrast, the hypothetic-deductivist picture fits better with the intervention studies which were indeed designed to test the hypotheses that H. pylori causes peptic ulcers and that ulcers can be cured by eradicating the bacteria with antibiotics. The logic of the experiment that Marshall et al. reported in 1988 was something like: If H. pylori causes ulcers, then antibiotic treatment of people with ulcers and H. pylori infection should cure the ulcers. The experimental design, however, made matters much more complex than this simple conditional allows. The antibiotic tinidazole did not by itself cure ulcers, because the bacteria quickly adapted to become resistant to it. The combination treatment of tinidazole+bismuth was much more effective, a generalization that Marshall and his colleagues made from this study. Hence they were being simultaneously hypothetic-deductivist and inductivist, using experiments to test hypotheses and also deriving new hypotheses by generalization from new experimental findings.
By "medical realism" I mean the view that diseases and their causes are real and that scientific investigation can gain knowledge of them. Medical realism is a species of scientific realism, which has been challenged from several directions, including empiricism, conceptualism, and social constructivism. Strict empiricists contend that scientific claims to truth should be restricted to observable phenomena (van Fraassen, 1980). Hence claims such as that bacteria exist in the stomach or that bacteria cause ulcers cannot be accepted as true, but at best as empirically adequate. Conceptualists conclude from the dramatic kinds of conceptual change that have taken place in the history of science that there is no legitmacy in a view of scientific investigation converging on the truth (Kuhn, 1970). Social constructivists maintain that scientific "facts" are social products arising from the interests and social networks of the participating scientists (Woolgar, 1988). However plausible anti-realism might be for exotic theories like quantum mechanics, the roles of instruments and experiments in the ulcers/bacteria case provides support for medical realism: ulcers and Helicobacter pylori are real independent of any mental and social constructions, and the theoretical claim that H. pylori is an important causal factor in ulcers can be accepted as true.
Empiricists can accept the reality of ulcers, since lesions are observable by the naked eye, and stomach ulcers were identified in autopsies long before the microsope was invented. But bacteria cannot be observed without a microscope. Van Fraassen (1980) denies that scientists see through a microscope: his strict empiricism would prevent him from accepting as true the claim that bacteria exist. More plausibly, Hacking (1983, ch. 11) notes that very difficult physical processes, such as diffraction of light for optical microscopes and electron transmission for electron microscopes, yield identical results, so that denying the reality of bacteria and other structures observed through microscopes would make the common results of the different physical processes a "preposterous coincidence". The thousands of articles published on H. pylori reflect their authors' experiences of observing bacteria through optical and electrical microscopes, experiences made even more shareable by published photographs such as figure 1. The empiricist has no grounds for elevating unaided sense experience above the observational practice of microscopists: like ordinary observation, microscopy is not error-free, but it has a high degree of reliability shown by intersubjective agreement. Helicobacter pylori can be seen, even if it takes a microscope to do so.
Conceptualism is sometimes a useful antidote to a too simple empiricism, when it recognizes that understanding the world goes well beyond sense experience; but it can err in the other direction by downgrading the role of experiment in scientific change. The relation of hypothesis and experiment is reciprocal, involving a kind of feedback loop in which experimental results suggest hypotheses and hypotheses suggest experiments and so on. Experimental data are not theory-independent, but they are not completely theory-dependent either. Endoscopy and microscopy revealed gastric spiral bacteria even to researchers who thought that Warren and Marshall were wrong. The conceptual structures described in Thagard (forthcoming-b) do not determine what researchers will detect with their instruments. Some of Marshall's experiments, for example the early attempt to develop an animal model of disease production by H. pylori, were not successful. Even more remarkably, some researchers who set out to refute his claims about the link between bacteria and ulcers produced experiments that confirmed those claims. Scientists' investigations of nature depend heavily on the conceptual structures with which they design experiments, but experiments often display a recalcitrance to expectations that cannot be explained if one thinks of nature only as a mental construction.
Similarly, it is implausible to view the bacterial theory of ulcers wholly as a social construction. As we will see below, there were many social processes such as collaboration, communication, and consensus that were important to the development and acceptance of the new ideas. But these social processes operated in concert not only with the psychological processes in the minds of researchers, but also in concert with physical processes by which scientists used instruments to interact with the world. Financial, ideological, medical, or other interests do not suffice to enable medical researchers to see whatever they want to see through a microscope or to obtain whatever biopsy samples they want to obtain with an endoscope. Using commonly accepted instrumental techniques and experimental methods, scientists achieved consensus in part because of physical interaction with a world not generated by their mental and social processes. Anyone who believes that H. pylori and the diseases it causes are pure social or mental constructions might receive a useful dose of reality by replicating Marshall's self-experiment.
Note that the emphasis on instrument and experiment in this paper is not a competing explanation for scientific change to the cognitive explanations given in Thagard (forthcoming-b). The use of instruments in observation and the design and conduct of experiments all depend on mental representations for diseases and microbes. Interacting with the world depends on thinking, just as thinking depends on interacting with the world.
In sum, the ulcers/bacteria case has several aspects that support a realist interpretation: reliability of instruments, experimental recalcitrance, and causal efficacy. Unless one accepts as true the claims that H. pylori inhabit the stomach and can cause ulcers, there is no plausible explanation of why so many scientists have been able to observe the bacteria with microscopes, of why experimenters sometimes do not get the results they want, and of why antibiotics are such an effective cure for many cases of ulcers.
Like most scientists, medical researchers do not spend most of their time theorizing. They devote immense efforts to designing, conducting, and analyzing the results of experiments. Scientific experiments often involve instruments of varying degrees of complexity, from the multi-billion dollar accelerators needed for research in high-energy physics to the multi-million dollar brain scanning devices increasingly used in neuroscience to the computers used by cognitive psychologists to measure reaction times. In all these fields, there is great epistemological significance in the recalcitrance of nature, which often fails to provide researchers with the experimental results they expect. This recalcitrance, and the role of instruments and experimental design in enabling researchers to manipulate natural occurrences, renders implausible any attempt to construe the world purely as a mental or social construction. Understanding scientific change requires paying attention not only to the minds and social interactions of scientists, but also to the physical activities by which they intervene in the world and extract information from it. The development and acceptance of the bacterial theory of ulcers depended crucially on the use of instruments such as microscopes and endoscopes that are needed to observe bacteria and ulcers, and also on a series of experiments that were required to show that there is a causal relation between H. pyloriinfection and gastric ulcers. Scientific change is equally a mental, physical, and social process.
I will now describe several social processes that are part of an explanation of how the theory that most peptic ulcers are caused by Helicobacter pylori came to be formed and eventually accepted. First, research in this area, like most current research is highly collaborative, involving multiple scientists working together. Second, spread of the new ideas about ulcers required their communication through the medical community by various means, including personal contact, conferences, and publications. Third, the growing consensus that ulcers are caused by bacteria is the result of various social processes, including a Consensus Development Panel meeting convened by the U.S. National Institutes of Health in 1994. I will also describe more briefly other social aspects of scientific change, including funding of medical research and the role of pharmaceutical companies.
A glance at science journals such as Nature, Science, and Physical Review Letters, shows that the vast majority of scientific papers today are co-authored, reflecting a variety of kinds of collaboration among scientists. Similarly, most medical research today is collaborative. For example, of the 44 research articles in the issues of The Lancet in July to September, 1995, only 1 is single-authored; and the average number of authors per article is greater than 7. Similarly, research on the bacterial theory of ulcers has been highly collaborative, as I will detail by describing the joint work of J. Robin Warren, Barry Marshall, and other researchers.
One obvious reason why scientists collaborate is that there are research projects that require more expertise than any one individual possesses. Robin Warren, a pathologist at Royal Perth Hospital, discovered gastric spiral bacteria in stomach biopsies in 1979, but was unable to investigate their clinical significance on his own, since that investigation required expertise in gastroenterology. In 1981, Barry Marshall was a trainee in internal medicine, and the chief of gastroenterology, Tom Waters, suggested that Marshall carry out clinical research on the medical significance of Warren's bacteria. This research required both gastroenterology, to identify cases of gastric disease and take biopsies, and pathology, to determine the presence or absence of bacteria in the biopsies.
The first publication on ulcers and bacteria by Warren and Marshall has a curious structure. Under a common title, "Unidentified Curved Bacilli on Gastric Epithelium in Active Chronic Gastritis", Lancet published two separate letters, one by Warren and one by Marshall (Warren and Marshall, 1983 ) (3). Warren's letter described work on the bacteria that he had conducted before beginning collaboration with Marshall. Subsequently, Marshall and Warren published several joint papers reflecting their continuing collaboration.
The 1982 study which first revealed an association between bacterial infection and peptic ulcers was a collaborative effort that required both gastroenterology and pathology (Marshall and Warren, 1984). At the end of this paper, Marshall and Warren (1984, p. 1314) thank a host of people who provided various kinds of assistance:
We thank Dr T. E. Waters, Dr. C. R. Sanderson, and the gastroenterology unit staff for the biopsies, Miss Helen Royce and Dr. D. I. Annear for the microbiology studies, Mr Peter Rogers and Dr L. Sly for supplying the G & C data, Dr. J. A. Armstrong for the electron microscopy, Dr. R. Glancy for reviewing slides, Miss Joan Bot for the silver stains, Mrs Rose Rendell of Raine Medical Statistics Unit UWA, and Ms Maureen Humphries, secretary, and, for travel support, Fremantle Hospital.
Notice the wealth of expertise required for the study: gastroenterology, microbiology, microscopy, statistics, etc. All of these specialties require years of intense training, so no individual researcher could have conducted the 1982 study alone.
Similarly, the 1984 attempt to fulfil Koch's postulates for bacteria and gastritis by Marshall's self-experiment required a team of researchers (Marshall, Armstrong, McGechie, and Clancy, 1985). This paper lists the specialties of the authors as follows:
Barry J. Marshall, registrar in microbiology,
David B. McGechie, microbiologist,
Ross J. Clancy, pathologist,
John A. Armstrong, electron microscopist.
Marshall's self-administration of bacteria would have been uninformative without the assistance of various specialists to help determine whether the bacteria had infected his stomach. That additional help was useful for this project is clear from the acknowledgments (Marshall et al., 1985, p. 439):
We wish to thank Dr J. R. Warren for advice on the historical aspects; Dr I. G. Hislop for performing the gastroscopies; Mr N. Nokes for the cultures; and S. H. Wee (EM) and J. E. Holdsworth for the histological preparations.
Whereas the 1982 experiment was done in one hospital, Perth Royal, the 1984 experiment required collaboration across two organizations. When it was conducted, Marshall, McGechie, and Clancy were all in the department of microbiology at Fremantle Hospital, while Armstrong was at Perth Royal. Note also how the need for collaborators often corresponds for the need for expertise with different instruments. This project needed gastroenterologists for expertise with gastroscopy, pathologists for expertise with microscopes, and microbiologists for expertise with stains and cultures, as well as an expert whose profession was defined by his instrument, the electron microscope.
The need for collaboration intensified with the studies begun in 1985 to determine whether eradication of bacteria is an effective treatment for duodenal ulcers. Marshall et al. (1988) has no fewer than nine co-authors drawn from four medical specialties: gastroenterology (Barry Marshall, Raymond Murray, Thomas E. Waters, Christopher R. Sanderson), microbiology (C. Stewart Goodwin, Elizabeth D. Blincow), histopathology (J. Robin Warren), and pharmacy (Stephen J. Blackbourn) (4). The acknowledgments thank several other personnel for help with endoscopies. The seven year follow-up to determine the long-term benefits of Helicobacter pylori eradication required a similarly broad range of kinds of expertise, although the researchers were different except for Warren and Marshall (Forbes et al., 1994). Clearly, experimental demonstration that antibiotics can cure ulcers required cooperation across medical specialties.
In Thagard (forthcoming-b) I cited five additional papers that provide convincing evidence that use of antibiotics to eradicate Helicobacter pylori cures gastric or duodenal ulcers. All five papers are co-authored, with an average of more than five authors per paper. For example, the researchers who have collaborated with Dr. David Graham (e.g. Graham et al., 1992) include epidemiologists, pediatricians, and pathologists as well as gastroenterologists. Remarkably, one paper that found an association between Helicobacter pylori infection and gastric cancer lists as its author "The EUROGAST Study Group", which has more than two dozen members spread across many countries and institutions (EUROGAST Study Group, 1993).
It is thus obvious that the research that produced the evidential support for the bacterial theory of ulcers is not the product of individual minds working in isolation, but required the cooperative work of many teams of scientists. Figure 3 shows some of the social connections that contributed to the work of Marshall and Warren, grouped according to co-authorship. Such interconnections are typical of research in the natural sciences, as well as in some social sciences such as psychology. Hence the interactions of researchers in producing and interpreting experimental research must be taken into consideration in any adequate account of scientific change.
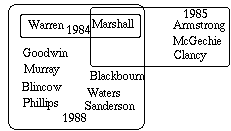
Figure 3. Research teams, as shown by the authorship of Marshall and Warren (1984), Marshall et al. (1985), and Marshall et al. (1988) (5).
Philosophy of science is concerned not only with how science is done, but also with how it should be done. My conclusions concerning the importance of collaboration to the ulcers/bacteria case are both descriptive and normative. Descriptively, we must notice that collaboration did occur; normatively, it is clear that scientific research concerning peptic ulcers and H. pylori would have been much less effective, efficient, and illuminating without collaborations among pathologists, gastroenterologists, microbiologists, and other personnel. As with much other research in contemporary science, collaboration not only facilitates scientific change, but is essential to it. See Thagard (forthcoming-a) for further normative analysis of collaboration.
Scientific change requires not only the production of research, but also its communication to other researchers. This section outlines the role played in the development and dissemination of the bacterial theory of ulcers by four kinds of communication: personal contacts, conferences, journals, and the public press.
The spread of new ideas often depends on personal interactions. In 1981, Barry Marshall heard about Robin Warren's observations of gastric spiral bacteria because Tom Waters, the chief of gastroenterology, suggested that Marshall help Warren investigate the bacteria. Personal contacts were also important in arranging the first international presentation of the results of the 1982 that first found an association between ulcers and bacteria. David McGechie, a microbiologist at Fremantle Hospital, had received an invitation to the International Workshop on Campylobacter infections, and suggested to Marshall that he submit his findings to that meeting (Marshall 1989). McGechie provided Marshall with the home telephone number of Martin Skirrow in Worcester, England. After a phone conversation, Marshall mailed Skirrow some isolates of the newly cultured bacteria.
Once the new ideas about bacteria and ulcers began to gain acceptance, the main researchers such as Barry Marshall and David Graham became in great demand for speaking engagements, another kind of personal contact. In 1996, Marshall was booked 18 months in advance for personal appearances (6).
The first public presentation of the results of the 1982 study was the local meeting of the Royal Australian College of Physicians in 1982 (Marshall, 1989). But Marshall's submission to the 1983 meeting of the Australian Gastroenterological Society was rejected. In contrast, Marshall's presentation at the International Workshop on Campylobacter infections in Brussels in 1983 prompted substantial interest in researchers from several countries.
Strikingly, the hypothesis that the gastric spiral bacteria caused ulcers had a much more positive initial reception from medical microbiologists than from gastroenterologists, who had pre-existing ideas about acidity as the major causal factor in ulcers. Marshall and Warren's (1984) report of their 1982 study was not immediately accepted by the editors of The Lancet, who had received negative referee reports. But as the result of the 1983 meeting in Brussels a number of microbiologists such as Martin Blaser began finding the bacteria in patients with gastritis and ulcers. The growing recognition of the importance of Marshall and Warren's research made gastroenterologists take it more seriously. Using a football analogy, we might describe the acceptance of the bacterial theory ulcers as a kind of "epistemic end run": a direct assault on gastroenterology was unsuccessful because of entrenched ideas in that field, but an indirect pursuit of the new ideas was possible via microbiology.
It must be recognized, however, that in the mid-1980s the evidence for the claim that H. pylori causes peptic ulcers was meager. Even gastroenterologists who were very interested in the new hypothesis viewed it as lacking in scientific support, and were annoyed by conference presentations that aggressively pushed the hypothesis in the absence of careful experiments that supported the causal claim. By the 1990s, however, such experiments had been done by various researchers, and conference discussion shifted from the question of whether H. pylori causes ulcers to how it does so and how it can be eradicated.
Warren and Marshall published their 1983 and 1984 communications, as well as the 1988 article on treatment of duodenal ulcers, in The Lancet, the most widely read British medical journal. The dramatic growth of interest in ulcers and bacteria is shown in figure 4, which shows that by 1989 there were well over 100 papers published on the topic. Most of the papers published in the 1990s providing substantial evidence that eradication of Helicobacter pylori cures peptic ulcers were published in The Lancet, although some also appeared in the New England Journal of Medicine and Annals of Internal Medicine (see Thagard forthcoming-b for references).
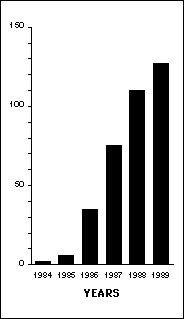
Figure 4. Growth in the number of journal articles on the role of Helicobacter pylori in peptic ulcer disease and gastritis, adapted from Science Watch, vol. 1, no. 4, p. 7, published by Institute for Scientific Information.
Unlike most scientific journals, medical journals such as The Lancet and The New England Journal of Medicine publish editorials along with research reports. The editorials allow experts in a field to comment on the clinical significance of recent findings. For example, David Graham (1993) wrote an editorial for The New England Journal of Medicine discussing recent studies and arguing that H. pylori infection is the most common cause of peptic ulcer and accounts for the majority of cases. Because such editorials are concise and less technical than research reports, they may have a substantial impact on belief change in medical researchers and physicians not directly involved with the topic.
Although in recent years the bacterial theory of ulcers has received enormous support in the medical journals, many physicians are still treating ulcer patients with traditional antacids. Communication of research results to physicians is often delayed, since many of them do not routinely read reports of clinical trials, but get their information indirectly through newsletters and drug company announcements. On the other hand, some patients have heard about the new results more quickly thanks to reports on Marshall's work that have appeared in the popular press, for example in The New York Times, The Washington Post, Consumer Reports, and the New Yorker. Television shows describing the breakthroughs have been broadcast in Australia, England, and Canada. Since peptic ulcers affect such a large proportion of the population (10%), it is not surprising that reports of a new cure have received popular attention. More surprising is the fact that in some cases patients have had to bring the new treatments to the attentions of their physicians rather than vice versa.
In most scientific fields, consensus evolves intangibly, as myriad scientists come to accept new hypotheses. Consensus may slowly become evident in the converging statements of review articles and textbooks, but there is no central social mechanism that produces a consensus. In medical research, the need for a consensus is much more acute, since hypotheses such as the bacterial theory of ulcers have direct consequences for the treatment of patients. In February, 1994, the U.S. National Institutes of Health (NIH) convened a conference in Washington, D. C. to examine the claim that peptic ulcers are caused by Helicobacter pylori .
Since 1977, NIH has conducted a Consensus Development Conference Program whose purpose is produce consensus statements on important and controversial statements in medicine. NIH's World Wide Web site describes the program as follows:
NIH Consensus Development Conferences are convened to evaluate available scientific information and resolve safety and efficacy issues related to biomedical technology. The resultant NIH Consensus Statements are intended to advance understanding of the technology or issue in question and to be useful to health professionals and the public.
NIH Consensus Statements are prepared by a non advocate, non-Federal panel of experts, based on (1) presentations by investigators working in areas relevant to the consensus questions during a 2-day public session; (2) questions and statements from conference attendees during open discussion periods that are part of the public session; and (3) closed deliberations by the panel during the remainder of the second day and morning of the third. This statement is an independent report of the panel and is not a policy statement of the NIH or the Federal Government (7).
The 1994 consensus development conference on Helicobacter pylori in peptic ulcer disease was the ninety-fourth sponsored by NIH.
In accord with NIH guidelines, this conference was organized around several groups of people. First a planning committee was established, chaired by Dr. Tadataka Yamada, Chair of the Department of Internal Medicine at the University of Michigan. The planning committee chair is required to be a knowledgeable and prestigious medical figure who is not identified with strong advocacy of the conference topic or with relevant research. The fifteen other members of the planning committee included researchers who were by then advocates of the bacterial theory of ulcers, including Martin Blaser, David Graham, and Barry Marshall, but it also included experts on digestive diseases who were not so directly involved. The consensus development panel consisted of fourteen people chosen for various kinds of expertise who were specifically not identified with advocacy or promotional positions with respect to the issues to be resolved by the conference.
Presentations to the panel were made by twenty-two researchers who were advocates for and against the claim that H. pylori are a causal factor in peptic ulcers. Martin Blaser, David Graham, and Barry Marshall were among those who argued for that claim, but more skeptical presentations had such titles as "Limitations of the Helicobacter pylori hypothesis" and "Current uncertainties about the impact of Helicobacter pylori on the complications of peptic ulcer disease." By 1994, however, the case for bacterial involvement in ulcers was strong, and most of the speakers at the consensus conference supported it. On February 9, 1994, the panel presented its statement concluding that ulcer patients with H. pylori infection require treatment with antimicrobial agents. This statement was later published in the widely read Journal of the American Medical Association (National Institutes of Health Consensus Development Panel, 1994).
The NIH panel was a formal version of a process that often happens informally in science, when relatively disinterested researchers can constitute a kind of jury for settling scientific controversies. For example, Kim (1994) describes how medical personnel provided a kind of neutral jury to evaluate disputes early in this century concerning the plausibility of Mendelian genetics, which had both advocates and critics. Similarly, the hypothesis proposed in 1980 that dinosaur extinction was caused by an asteroid striking the earth had vehement advocates and critics; but there were also many informed members of the scientific community who were not directly involved in the controversy and who were sufficiently well informed to provide objective assessment of the evidence. Science benefits both from diversity of approaches, when some researchers pursue new ideas even when there is limited empirical support for them, and from the social process by which researchers with no stake in or against those ideas provide an informed evaluation of them.
The 1994 NIH conference was only one of the social mechanisms that encouraged increased acceptance of the bacterial theory of ulcers. Some researchers and physicians learned about the emerging evidence for the theory from conferences, journals, and personal contacts. Consensus is by no means universal: John Graham (1995) rejects the claim that H. pylori has been shown to be the primary cause of peptic ulcers. As of 1996, many physicians are still treating patients with antacids instead of antibiotics.
The social processes that in part produce scientific change involve organizations as well as individuals. In medical research, the American NIH plays a direct role in encouraging consensus about treatments, but other organizations were important in the earlier development of the bacterial theory of ulcers, which depended on hospitals, universities, drug companies, and other funding agencies.
Warren and Marshall's initial collaboration took place at the Royal Perth Hospital, where Warren was a pathologist and Marshall a trainee in internal medicine. Their early research does not cite any special funding sources, but was done with the resources of the Royal Perth and Fremantle Hospitals (Warren and Marshall 1983, Marshall and Warren 1984, Marshall et al. 1985). Subsequent larger-scale trials required greater resources, and the 1985-1987 research on eradication of H. pylori received funds from the National Health and Medical Research Council of Australia, the Royal Perth Hospital General Fund, Gist Brocades, and Pfizer (Marshall et al. 1988). After Marshall left Australia in 1986, his research was conducted at the University of Virginia Health Sciences Center. Today (1996), his World Wide Web page includes a disclaimer that indicates he consults with and accepts honoraria from Astra-Merck, Abbott, Glaxo-Wellcome, Eli-Lilley, Pfizer, Procter and Gamble and many other medical companies. In addition, he holds stock in several pharmaceutical and diagnostic companies, and has an interest in Tri-Med Specialties Inc. and Meretek, which are companies developing urea breath tests for H. pylori.
Clinical trials are very expensive, and usually require funding by pharmaceutical companies that have an interest in showing that a new drug is effective. Bradley (1993, p. 153) reports a survey that found that 89% of trials which were supported by the pharmaceutical industry had positive results in favor of a new treatment, but only 61% of trials not so supported found positive results. Because H. pylori infections can be cured with combinations of generic antibiotics in which no drug company has a proprietary interest, funding for research on this topic has been primarily obtained from other sources. Many of the early experiments on ulcers and H. pylori were done by interested researchers using funds redirected from other projects. The makers of Zantac and Tagamet, two of the most lucrative drugs ever produced, have an interest against the new treatment of ulcers which can actually eradicate the disease, but the drug companies mounted no resistance to the new theory of ulcers. Zantac and Tagamet have recently become available in the U.S. without a prescription, allowing people with gastric distress to alleviate their symptoms without consulting physicians concerning the possible presence of H. pylori infections. In the U.S., pharmaceutical companies have recently received approval for drugs that combine antacid and antibiotic treatments. These should make it easier for physicians to know what to prescribe to their ulcer patients.
In the U.S. and Canada, conservative government funding agencies were slow to appreciate the medical importance of Helicobacter pylori. The role of H. pylori in ulcers, gastric cancer, and other diseases is a socioeconomic issue as well as a medical one, since government health providers stand to save substantial amounts of money by eradicating H. pylori rather than pursuing traditional antacid treatment (O'Brien, Goeree, Mohamed, and Hunt, 1996).
My account of the social processes affecting the new theory of ulcers is incompatible both with traditional philosophy of science, which tends to ignore the social altogether, and with modern sociology of science, which tends to give the social an exclusive role in explaining scientific change. Philosophy of science claims to reach normative conclusions about how science should be done, but philosophical research informed by history and psychology shows how descriptive studies can inform normative conclusions (Thagard 1988, ch. 7). Similarly, descriptive studies of the social contributors to scientific development can feed into normative conclusions. It is obvious, for example, that collaboration was a positive contributor to the emergence of the bacterial theory of ulcers, since the crucial experimental studies could not have been performed without combining the expertise of gastroenterologists, pathologists, microbiologists, and others. Normatively, therefore, we can conclude that collaboration is a social process that contributes to the development of scientific knowledge. Another contributor is the organization of the NIH consensus development conferences, when a panel of experts with no special interests in the issue convenes to hear diverse presentations and reach an impartial recommendation about treatment. As sociologists have pointed out, scientists approach their research with diverse interests and social contexts that undoubtedly affect their work, but institutions such as the NIH panel provide a relatively impartial forum for evaluating competing claims. The panel is a more concentrated and organized form of what takes place in journals through the procedure of peer review.
While noticing the importance of social processes such as collaboration, communication, consensus, and funding to scientific research, it is important not to succumb to the slogan that science is a social construction. Proponents of that slogan tend to ignore both the psychological processes of theory construction and acceptance that I described in Thagard (forthcoming-b), and the physical processes of interaction with the world via instruments and experiments that I described in sections 1-2 of this paper. Undoubtedly interests and social networks abound in the ulcers case as in other episodes in the history of science. But explaining scientific change solely on the basis of social factors is as patently inadequate as purely logical and psychological explanations.
Latour (1988, p. 229) says that science is politics by other means. He depicts research as a Machiavellian series of trials of strength in which scientists attempt to recruit allies to vanquish their foes. A Latourian history of the bacterial theory of ulcers would ignore the cognitive processes of scientists, since Latour (1988, p. 218) says that we do not think, only write. It would also misconstrue the role of instruments and experiments, as when Latour (1988, p. 73) explains Pasteur's laboratory work by saying: "To win, we have only to bring the enemy to where we are sure we will be the stronger. A researcher like Pasteur was strongest in the laboratory." This is nonsense; microbiologists go to the laboratory because it enables them to study organisms under controlled conditions with the appropriate instruments. Of course, science does have a political side, evident in the operations of funding agencies, consensus panels, and other social operations such as Marshall's working with microbiologists in the face of opposition from many gastroenterologists. But science also has cognitive and experimental sides that must figure in explanations of scientific change.
What causes scientific change? This question is clearly at least as complex as asking: What causes ulcers? In the latter case, although the eradication studies show that H. pylori infection is probably the most important cause of peptic ulcers, a full account of the aetiology of ulcers has to take into account a wealth of other factors that help to explain why only some of the people with bacterial infections get ulcers. Future research on the operation of the digestive and immune systems should start to fill in some of the answers. Already the causal mechanisms by which H. pylori produce ulcers are becoming better understood (e.g. Olbe et al., 1996). Similarly, a complex of psychological, physical, and social mechanisms were responsible for the development and acceptance of the bacterial theory of ulcers. One of the most important, I contend, is the psychological process of assessment of explanatory coherence described in Thagard (forthcoming-b). Scientific change is in part change in scientists minds, and explanatory coherence provides the most psychologically and historically plausible account of belief revision now available. But a fuller view of the causes of scientific change is suggested by figure 3, which depicts mind, nature, and society as interacting causal influences on the development of science.
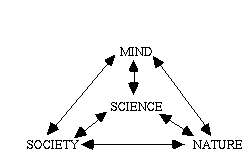
Figure 5. Science as a complex system. Arrows indicate mutual causal influences. Reprinted from Thagard (1995).
Although it has been convenient to organize this paper and its companion in terms of mind, nature, and society, we must not forget the interactions among these elements. Mind affects nature through the mental processes crucial to the use of instruments and the design of experiments, at the same time as nature affects mind by producing observations and experimental results which may or may not conform with expectations. Society affects mind through the goals and interests that motivate scientists and through the organizations and social networks that make modern science possible, at the same time as mind affects society when organizations are affected by the discoveries of individuals (8). Society affects nature through the contributions of needs, organizations, and networks to experimental research, at the same time as nature affects society when scientific organizations contribute to new discoveries arising from interactions with the world.
In accord with figure 3, my account of the emergence in the past decade and a half of major new views about the causes of ulcers has described science as a complex system. The system is simultaneously: psychological (involving individual scientists' cognitive processes for discovery and acceptance), physical (requiring scientists to interact with the natural world using instruments and experiments), and social (involving the interaction of scientists with each other). Only by attending to all these aspects of the growth of knowledge can we fully explain scientific change.
*This research is supported by a grant from the Social Sciences and Humanities Research Council of Canada. I am grateful to Drs. Barry Marshall, David Graham, Richard Hunt, J. Robin Warren, and Tadataka Yamada for helpful conversations.
(1) For details on how the urea breath test works, see the World Wide Web page of Barry Marshall's Helicobacter Foundation: http://www.helico.com/.
(2) This paper has nine authors. See section 5 below for details of the nature of the collaboration between members of several different medical specialties.
(3) The two letters are usually cited as one publication. Goodwin and Worsley (1993, p. 3) state that the unusual format was suggested by the electron microscopist J. A. Armstrong because Warren and Marshall could not agree on the wording of a joint letter. However, according to Warren (personal communication), the letters were kept separate because the first one reflected work he had done alone; the second letter, which lists Marshall as author, described joint work. Marshall (personal communication) reports that the two-letter format was suggested by the Lancet editor who thought that an original single letter was too long.
(4) The ninth researcher, Michael Phillips, is listed as being at Curtin University in Perth.
(5) In the terminology of social network analysis, collaboration can be understood as a kind of affiliation network, and figure 1 can be interpreted as a hypergraph (Wasserman and Faust, 1994). A much more complicated graph would be needed to display all of the relevant collaborations.
(6) See Marshall's World Wide Web page: http://www.vianet.net.au/~bjmrshll/.
(7) Source: Web page: http://text.nlm.nih.gov/nih/upload-v3/About/about.html.
(8) One aspect of mind that I have neglected in these papers is personality.
Personal characteristics such as aggressiveness, tenacity, and conservatism
were undoubtedly of some importance in the roles that different researchers
played. This case does not support the claim that scientific change is primarily
supported by later borns, since Warren and Marshall are both eldest children.
Ackermann, R. J. (1985). Data, instruments, and theory. Princeton: Princeton University Press.
Bradbury, S. (1968). The microscope past and present. Oxford: Pergamon.
Bradley, G. W. (1993). Disease, diagnosis, and decisions. Chichester: John Wiley & Sons.
Bulloch, W. (1979). The history of bacteriology. New York: Dover.
Cutler, A. F., Havstad, S., Ma, C. K., Blaser, M. J., Perez-perez, G. I., & Schubert, T. T. (1995). Accuracy of invasive and noninvasive tests to diagnose Helicobacter pylori infection. Gastroenterology, 109, 136-141.
Dobell, C. (1958). Antony von Leeuwenhoek and his 'little animals'. New York`: Russell & Russell.
EUROGAST Study Group (1993). An international association between Helicobacter pylori infection and gastric cancer. Lancet, 341(8857), 1359-1362.
Forbes, G. M., Glaser, M. E., Cullen, D. J. E., Warren, J. R., Christianson, K. J., & Marshall, B. J. (1994). Duodenal ulcer treated with Helicobacter pylori eradication: Seven year follow-up. Lancet, 342, 258-260.
Galison, P. (1987). How experiments end. Chicago: University of Chicago Press.
Gooding, D. (1990). Experiment and the nature of meaning. Dordrecht: Kluwer.
Goodwin, C. S., & Worsley, B. W. (1993). The Helicobacter genus: The history of H. pylori and taxonomy of current species. In C. S. Goodwin & B. W. Worsley (Eds.), Helicobacter pylori: Biology and clinical practice (pp. 1-13). Boca Raton: CRC Press.
Graham, D. Y. (1993). Treatment of peptic ulcers caused by Helicobacter pylori. New England Journal of Medicine, 328, 349-350.
Graham, J. R. (1995). Helicobacter pylori: Human pathogen or simply an opportunist? Lancet, 345, 1095-1097.
Graham, D. Y., Klein, P. D., & Evans, D. J. e. a. (1987). Campylobacter pylori detected non-invasively with the 13C-urea. Lancet, 1, 1174-1177.
Graham, D. Y., Lew, G. M., Klein, P. D., Evans, D. G., Evans, D. J., Saeed, Z. A., & Malaty, H. M. (1992). Effect of treatment of Helicobacter pylori infection on long-term recurrence of gastric or duodenal ulcer: A randomized, controlled study. Annals of Internal Medicine, 116, 705-708.
Hacking, I. (1983). Representing and intervening. Cambridge: Cambridge University Press.
Hennekens, C. H., & Buring, J. E. (1987). Epidemiology in medicine. Boston: Little, Brown.
Hirschowitz, B. I. (1993). Development and application of endoscopy. Gastroenterology, 104, 337-342.
Hopkins, H. H., & Kapany, N. S. (1954). A flexible fiberscope using static scanning. Nature, 173, 39-41.
Kim, K. (1994). Explaining scientific consensus: The case of Mendelian genetics. New York: Guilford.
Kuhn, T. (1970). Structure of scientific revolutions (2 ed.). Chicago: University of Chicago Press.
Latour, B. (1988). The pasteurization of France (Sheridan, A. and Law, J., Trans.). Cambridge, MA: Harvard University Press.
Marshall, B. J. (1989). History of the discovery of C. pylori. In M. J. Blaser (Eds.), Campylobacter pylori in gastritis and peptic ulcer disease (pp. 7-22). New York: Igaku-Shoin.
Marshall, B. J., Armstrong, J. A., McGechie, D. B., & Clancy, R. J. (1985). Attempt to fulfil Koch's postulates for pyloric campbylobacter. Medical Journal of Australia, 142, 436-439.
Marshall, B. J., Goodwin, C. S., Warren, J. R., Murray, R., Blincow, E. D., Blackbourn, S. J., Phillips, M., Waters, T. E., & Sanderson, C. R. (1988). Prospective double-blind trial of duodenal ulcer relapse after eradication of campylobacter pylori. Lancet, 2(8626/8627), 1437-1441.
Marshall, B. J., Plankey, M. W., Hoffman, S. R., Boyd, C. L., Dye, K. R., Frierson, H. f., Guerrant, R. L., & McCallum, R. W. (1991). A 20-minute breath test for Helicobacter pylori. American Journal of Gastroenterology, 86, 438-445.
Marshall, B. J., & Warren, J. R. (1984). Unidentified curved bacilli in the stomach of patients with gastritis and peptic ulceration. Lancet, 1(8390), 1311-1315.
National Institutes of Health Consensus Development Panel (1994). Helicobacter pylori in peptic ulcer disease. Journal of the American Medical Association, 272, 65-69.
O'Brien, B., Goeree, R., Mohamed, H., & Hunt, R. (1996). Cost-effectiveness of Helicobacter pylori eradication for the long-term management of duodenal ulcer in Canada. Archives of Internal Medicine, 155, 1958-1964.
Olbe, L., Hamlet, A., Dalenbäck, J., & Fändriks, L. (1996). A mechanism by which Helicobacter pylori infection of the antrum contributes to the development of duodenal ulcer. Gastroenterology, 110, 1386-1394.
Steer, H. W., & Colin-Jones, D. G. (1975). Mucosal changes in gastric ulceration and their response to carbenoxolone sodium. Gut, 16, 590-597.
Thagard, P. (1988). Computational philosophy of science. Cambridge, MA: MIT Press/Bradford Books.
Thagard, P. (1995). Explaining scientific change: Integrating the cognitive and the social. In D. Hull, M. Forbes, & R. Burian (Eds.), PSA 1994, vol. 2 (pp. 298-303). East Lansing, MI: Philosophy of Science Association.
Thagard, P. (forthcoming-a). Collaborative knowledge. Noûs.
Thagard, P. (forthcoming-b). Ulcers and bacteria I: Discovery and acceptance.
van Fraassen, B. (1980). The scientific image. Oxford: Clarendon Press.
Warren, J. R., & Marshall, B. J. (1983). Unidentified curved bacilli on gastric epithelium in active chronic gastritis. Lancet(8336), 1273-1275.
Wasserman, S., & Faust, K. (1994). Social network analysis: Methods and applications. Cambridge: Cambridge University Press.
Woolgar, S. (1988). Science: The very idea. Chichester, Sussex: Ellis Horwood. EUROGAST Study Group (1993). An international association between Helicobacter pylori infection and gastric cancer. Lancet, 341(8857), 1359-1362.